
Absolute surgical indications often quoted include: 1) open fractures 2) complete displacement of fracture ends with fragments greater than the width of the clavicular bone 3) clavicle shortening more than 2cm or with an angulation of more than 30 degrees. Essentially, these classifications broadly classify them into non-displaced fractures (AO/OTA classification type A) which can be managed conservatively, while management for displaced fractures (AO/OTA classification type B) remains controversial. Midshaft clavicular fractures can be classified by the Neer Classification or AO classification for risk stratification and management. The middle third of the clavicle is especially vulnerable to traumatic injury since it is the thinnest part of the clavicle without reinforcement protection by muscle and ligamentous attachments. It is a common injury among young adults with over one-third of all clavicular fractures occurring in adolescent male, and one-fifth in adolescent female. Midshaft clavicular fracture occupies 2.6–4% of all adult fractures. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.ĭata Availability: All information can be readily accessible on databases described on the manuscript (Pubmed, Embase, Medline, Cochrane).įunding: The author(s) received no specific funding for this work.Ĭompeting interests: The authors have declared that no competing interests exist. Received: DecemAccepted: ApPublished: April 29, 2022Ĭopyright: © 2022 Yan et al. PLoS ONE 17(4):Įditor: Osama Farouk, Assiut University Faculty of Medicine, EGYPT (2022) Operative management of midshaft clavicle fractures demonstrates better long-term outcomes: A systematic review and meta-analysis of randomised controlled trials. Surgical outcome is independent of fixation with plates or intra-medullary nails.Ĭitation: Yan MZ, Yuen W-s, Yeung S-c, Wing-yin CW, Wong SC-y, Si-qi WW, et al. Any child with a suspected posterior SC joint dislocations should be referred to the on-call orthopaedic team – these are orthopaedic emergencies, with CT angiograms favoured to characterise the extent of vascular injury and operative reduction performed, often in consultation with vascular surgeons.Of the 3094 patients of mean age 36.7 years in the 31 selected studies, surgical intervention was associated with improved DASH score (standard-mean difference SMD -0.22, 95% CI -0.36 to -0.07, p = 0.003 mean difference MD -1.72, 95% CI -2.93 to -0.51, p = 0.005), CMS (SMD 0.44, 95% CI 0.17–0.72, p = 0.001 MD 3.64, 95% CI 1.09 to 6.19, p = 0.005), time to union (non-adjusted SMD -2.83, 95% CI -4.59 to -1.07, p = 0.002 adjusted SMD -0.69, 95% CI -0.97 to -0.41, p24 months SMD -4.24, 95% CI -7.03 to -1.45, p = 0.003) and CMS (>24 months, SMD 1.03, 95% CI 0.39 to 1.68, p = 0.002 MD 5.77, 95% CI 1.63 to 9.91, p = 0.006). SC joint dislocations are classified as Grades I-V, with Grade V being a posterior dislocation. Hoarseness could indicate a recurrent laryngeal nerve injury or airway compromise. A dislocation may impact the structures behind including the trachea and blood vessels in that region. Posterior dislocations can present with pain over the anterior chest, increased on shoulder movement. If there is no evidence of medial epiphyseal fracture but pain and swelling is present you must consider a dislocation. 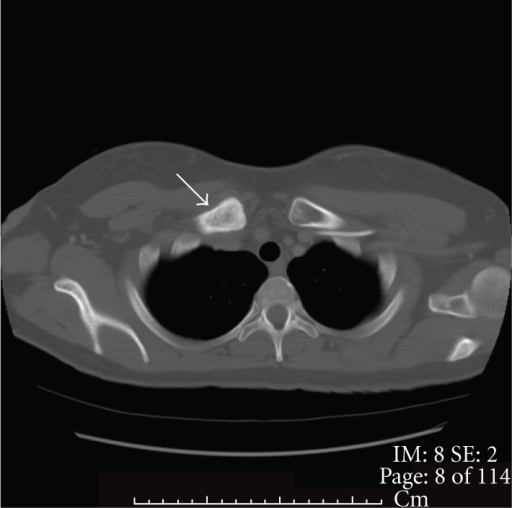 
Much less often the clavicle moves posteriorly in relation to the sternum, especially in the setting of tremendous force applied to the shoulder or the medial clavicle. Most children with an anterior SC joint dislocation can be managed with a sling or collar and cuff.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
